Quick Reference
Partners for
Opioid Safety
Opioids911-Safety is
recommended by...

American Academy of
Pain Management
![]()
American Association
for the Treatment of
Opioid Dependence

American Chronic Pain
Association
![]()
American College of
Apothecaries
![]()
American Society for
Pain Management
Nursing
![]()
National Association
of Drug Diversion
Investigators

National Fibromyalgia
& Chronic Pain
Association
![]()
National Fibromyalgia
Association

Reflex Sympathetic
Dystrophy Syndrome
Association

The Foundation for
Peripheral Neuropathy

TNA-The Facial Pain
Association
Certifications
We comply with the
HONcode Standard
for trustworthy health
information.
![]()
Verify Here
WMA Certified

Verify Here
Opioids911-Safety has been independently developed with support provided in part by educational grants from...
Purdue Pharma L.P.
2. What are safety concerns with opioids?
- How should I take my opioid pain relievers?
- How can opioids be harmful?
- What should I know and do about side effects?
- Could I become addicted to opioids?
- What is an opioid treatment agreement?
- What opioid prescribing restrictions should I know about?
A. How should I take my opioid pain relievers?
For safety's sake, opioid pain relievers must be taken exactly as you are told by the healthcare provider who prescribed the medicine. There also should be directions on the product container label and in any other information that comes with your prescription. It is very important that you read all information carefully, even if you have used the same or a similar opioid medicine in the past.
You must never take more of the opioid medicine than you are instructed, and never take it more often. If you think you are either not getting enough medicine or that the dose is too much, call your healthcare provider or pharmacist before changing the dose or how often you take the medicine.
 CAUTION: You must never chew, cut, crush, or dissolve opioid tablets, or open opioid capsules, unless specifically instructed to do so. Opioid patches must never be cut or folded, and they need to stick to the skin completely. Remove the old patch before putting on a new one, and never put heat over patches. If you are prescribed an opioid liquid, ask the pharmacist for a device to accurately measure each dose.
CAUTION: You must never chew, cut, crush, or dissolve opioid tablets, or open opioid capsules, unless specifically instructed to do so. Opioid patches must never be cut or folded, and they need to stick to the skin completely. Remove the old patch before putting on a new one, and never put heat over patches. If you are prescribed an opioid liquid, ask the pharmacist for a device to accurately measure each dose.
 It can take some time before pain-relieving effects of opioids begin. So, it can be important that you continue taking the prescribed dose of medicine every day and at the right time. Do not put off taking a regularly scheduled dose just because the pain is not troubling you at the moment.
It can take some time before pain-relieving effects of opioids begin. So, it can be important that you continue taking the prescribed dose of medicine every day and at the right time. Do not put off taking a regularly scheduled dose just because the pain is not troubling you at the moment.
CAUTION: What if you forget to take a dose?
If you forget to take a dose of oral or liquid opioid medicine at the correct time, do one of the following:
- If it is still close to the time when you were supposed to take it, then take the regular dose;
- If it is closer to when you should take your next dose, then wait until that time and take the regular dose on schedule. Never take doses close together or double the dose to make up for one that you missed.
If in doubt, call your healthcare provider. In the U.S., you also can call the National Poison Hotline at 1-800-222-1222.
If your pain worsens and the opioid medicine is not helping, talk to your opioid prescriber about a change of dose or a different opioid. Remember, however, that the goal of opioid therapy is to ease your pain enough so that you can be more comfortable and remain active. Becoming completely pain free all day long is usually not possible and cannot be expected.
If you take an opioid pain reliever regularly for a week or longer, do not suddenly stop taking it. This might cause uncomfortable feelings of opioid withdrawal (discussed below). When you are almost finished with opioid therapy your healthcare provider will slowly and safely decrease your dose a little at a time.
B. How can opioids be harmful?
Opioid medicines can be very harmful if they are not used as directed. Even when used correctly, caution is needed. The amount of an opioid can build up in the body, especially when it is first started or there is a change in dose or medicine. This can lead to problems, which do not always happen but are of concern.
WARNING: Opioids can cause overdose and death if they are not used correctly. They also can do serious harm, possibly causing death, if they are taken by adults, children, or pets for whom they were not prescribed.
 The most serious potential harm from opioids is trouble with breathing, called "respiratory depression." A person's breathing can become slow and so weak that he/she does not get enough oxygen. Their lungs may fill with fluid or the person might inhale and choke on their own saliva or vomit, causing worse breathing problems. Action must be taken quickly or the person may pass out, stop breathing, and their heart can stop beating.
The most serious potential harm from opioids is trouble with breathing, called "respiratory depression." A person's breathing can become slow and so weak that he/she does not get enough oxygen. Their lungs may fill with fluid or the person might inhale and choke on their own saliva or vomit, causing worse breathing problems. Action must be taken quickly or the person may pass out, stop breathing, and their heart can stop beating.
Fortunately, respiratory depression does not usually happened suddenly - it takes some time to develop. There are early warning signs of too much opioid, or "overmedication," that you and your caregivers - family or friends who look after you - can watch for. If respiratory depression gets worse, your caregivers can recognize if you are suffering from life-threatening opioid poisoning, or "overdose" - if they know what to look for.
Here is what to watch for in each condition (share this with your caregivers and you, too, should be familiar with this in case someone swallows your opioid medicine):
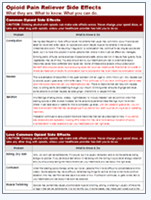
Signs to Watch For - Overmedication or Overdose?
|
Overmedication Warning - Call Healthcare ProviderU.S. residents also can call the National Poison Hotline at 1-800-222-1222. |
|
Overdose Poisoning - Call Emergency ServicesDial 911 in the U.S. or Canada; 112 or 999 in England or the European Union; or other numbers depending on your location. |
|
REMEMBER: If there are signs of overmedication, stop taking the opioids and call for instructions on what to do. If there are signs of overdose, call emergency services for help - right away.
WARNING: If a child or pet ever swallows an opioid that was not prescribed for them, it is always an emergency. Call for help immediately.
Opioids can especially cause respiratory depression in the elderly or persons who already have breathing problems, such as from asthma, chest congestion or infection, or during sleep, called "sleep apnea" (see below). When opioids are being prescribed, be sure to tell your healthcare provider if you have any breathing trouble.
How can you know if you might have sleep apnea?
 Take the following quiz, answering "yes" or "no" to each question:
Take the following quiz, answering "yes" or "no" to each question:
- Do you snore loudly almost every night?
- Have you ever been told that you gasp or stop breathing during sleep?
- Do you feel tired or groggy when you wake up in the morning
- Do you often wake up with a headache?
- Do you usually feel tired or worn out during the day?
- Do you fall asleep while sitting, reading, watching TV, or driving?
- Do you often have trouble remembering things or concentrating?
If you answered "yes" to one or more questions you may have sleep apnea. If you also are overweight, have a large neck, and/or have high blood pressure your risk of having sleep apnea is even greater. Talk to your opioid prescriber about your sleep problems before starting opioids.
[Based on "Snore Score™" from the American Sleep Apnea Association, 2008]
CAUTION: If possible, you should start taking a new opioid medicine, or first take any prescribed dose increase, during the day when you will be awake and other persons are around to see how you react to the medicine.
After awhile, as your body gets used to the daily opioid dose, respiratory depression becomes less likely to occur. This could take days or weeks, depending on the type of opioid and the dose. Meanwhile using alcohol or taking medicines sometimes called "downers" - like sedatives, tranquilizers, sleeping pills - or other drugs can combine with opioids in ways that slow breathing enough to be harmful. For safety's sake, you must tell the opioid prescriber about all substances or medicines that you take (or will be taking) with opioids.
CAREGIVER NOTE: Your loved one or friend taking opioids should be watched closely, even during sleep, for at least several days or longer when opioids are started or there is a change of dose or medicine. At the first sign of trouble - for example, if the person is constantly nodding off to sleep, or breathing or snoring strangely during sleep - wake them up and keep him/her awake; never let the person just "sleep it off." Call their healthcare provider for advice on what to do. If you cannot reach the provider, call the National Poison Hotline at 1-800-222-1222 (in the U.S.) or local emergency services for instructions.
C. What should I know and do about side effects?
 As with any medicine, opioids may produce some unpleasant feelings, or symptoms, and other bothersome conditions called "side effects." These do not always happen to everyone taking opioids or to the same extent. In some persons, however, they can be troubling. Fortunately, most side effects go away once you become used to taking opioids. Or, very often, a balance can be achieved between effective pain relief and minor side effects so that opioid therapy can be continued for as long as necessary.
As with any medicine, opioids may produce some unpleasant feelings, or symptoms, and other bothersome conditions called "side effects." These do not always happen to everyone taking opioids or to the same extent. In some persons, however, they can be troubling. Fortunately, most side effects go away once you become used to taking opioids. Or, very often, a balance can be achieved between effective pain relief and minor side effects so that opioid therapy can be continued for as long as necessary.
![]() For a complete list of side effects and what to do about them <click here>.
For a complete list of side effects and what to do about them <click here>.
A few opioid side effects are common, including:
 Constipation - irregular or difficult bowel movements. Diet and exercise can help and there are medicines to help relieve constipation. Ask your opioid prescriber or pharmacist. If you already have constipation, be sure to mention this when opioids are being prescribed for you.
Constipation - irregular or difficult bowel movements. Diet and exercise can help and there are medicines to help relieve constipation. Ask your opioid prescriber or pharmacist. If you already have constipation, be sure to mention this when opioids are being prescribed for you.- Nausea - a sensation of discomfort in the upper stomach with an urge to vomit ("throw up"). If you do vomit and cannot hold down your medicine, contact your opioid prescriber.
 Sedation - feeling mildly dizzy, drowsy, "cloudy-headed," or "in a fog." However, if you cannot stay awake or feel intoxicated, this may signal more serious opioid overmedication or overdose (described above).
Sedation - feeling mildly dizzy, drowsy, "cloudy-headed," or "in a fog." However, if you cannot stay awake or feel intoxicated, this may signal more serious opioid overmedication or overdose (described above).
Less often some patients taking opioids may experience itching, dry skin, confusion, muscle twitching or shaking, sweating, dry mouth, weakness, fatigue, or headaches. Also, if opioids are taken for a long time, they may decrease levels of certain hormones in men and women. This may reduce sex drive and sexual performance, and influence weight gain or depression ("feeling blue"), weaken bones, and cause menstrual period irregularities.
In rare cases certain opioid pain relievers may affect normal heartbeat or cause problems with urinating (peeing). After opioids are taken for awhile, the medicine may seem to actually make pain worse in some persons, but there also could be other reasons if this happens. Few persons have a true allergy to opioids; however, if a rash, hives, swelling, or tightening in the throat develops seek medical attention right away.
NOTE: It is important to know that drinking alcohol can make opioid side effects worse and be harmful. However, when taken as directed, opioid pain relievers themselves do not do any permanent damage to the body. Side effects go away if opioids are stopped or, in most cases, they can be treated so they are not as bothersome while continuing to take opioids.
For women, if you are pregnant or plan to become pregnant you must tell your opioid prescriber. Opioid medicines cross the placenta and enter the developing baby, so special care is needed during and after birth of the baby. Also, talk to your opioid prescriber before breastfeeding while taking opioids, since there will be small amounts of opioids in the breast milk.
![]() NOTE: If you are concerned about any unusual side effects, you can report them to the U.S. FDA by calling 1-800-FDA-1088, or at the FDA website by <clicking here>.
NOTE: If you are concerned about any unusual side effects, you can report them to the U.S. FDA by calling 1-800-FDA-1088, or at the FDA website by <clicking here>.
D. Could I become addicted to opioids?
Patients taking opioids as directed to relieve pain seldomly become addicted to the medicines. Addiction, itself, is a brain disease - both physical and mental - that requires special treatment.
 Addiction most commonly develops when a person misuses, or abuses, opioid drugs. That is, the person takes opioids more for the mind-altering effects they produce - such as to feel "high," calm or relaxed, or in a "good mood" - than for pain relief. After awhile, if the person tries to cut back or to quit misusing the opioids, it causes uncomfortable feelings both physically and mentally. This can lead to overpowering cravings or urges to take more opioids.
Addiction most commonly develops when a person misuses, or abuses, opioid drugs. That is, the person takes opioids more for the mind-altering effects they produce - such as to feel "high," calm or relaxed, or in a "good mood" - than for pain relief. After awhile, if the person tries to cut back or to quit misusing the opioids, it causes uncomfortable feelings both physically and mentally. This can lead to overpowering cravings or urges to take more opioids.
Once addicted, the person cannot stop misusing opioids - he/she loses control, even though this is not helping their pain and is ruining their lives. For example, they may avoid personal responsibilities or social activities to focus on getting and misusing opioids. This usually leads to trouble at work or school and at home.
Persons prescribed opioids for pain relief who have had problems with substance misuse or addiction in the past, including alcoholism, are at the greatest risk for developing addiction to opioid medicines. If you have had such problems it is very important that you tell any healthcare provider prescribing opioids for your pain, so you can be properly treated and get additional help if needed.
CAUTION: In a patient suffering both pain and addiction, the pain usually cannot be relieved unless the addiction is brought under control. So, pain can only be effectively treated, with opioids or other therapy, if the patient is honest with their opioid prescriber about past or present problems with drug misuse or addiction. In some cases, opioid prescribers may want to ask caregivers to provide helpful information about the patient's drug-using history (with the patient's permission).
Addiction is often confused with so-called "physical dependence," which consists of opioid tolerance and withdrawal. These effects may naturally occur in any person taking opioids and are not the same thing as addiction.
- Opioid Tolerance - may develop after some time as your body gets used to the opioid medicine. The opioid may not seem to provide the same amount of pain relief after you develop "tolerance" to it. This does not always happen but, in some cases, you may need to take more of the opioid or take it more often, or a different opioid can be tried. However, you should never change the way you take the medicine on your own without first talking to your opioid prescriber.
Opioid tolerance also can be a good thing. Over time, there is less concern about possible opioid effects on breathing and you also will better tolerate any bothersome side effects, like nausea, drowsiness, and others. Constipation is the one common side effect that may continue, so you should ask about this in advance when you are given an opioid prescription. -
Withdrawal - also may occur naturally after you get used to having a steady amount of opioid medicine in your body to feel and function well. If the amount of opioid medicine is quickly decreased or suddenly stopped entirely you may feel effects of opioid withdrawal.
 For advice on how to deal with emergency opioid withdrawal if you are running out of medicine or cannot get prescription refills after a hurricane, flood, earthquake, fire, or other disaster <click here>.
For advice on how to deal with emergency opioid withdrawal if you are running out of medicine or cannot get prescription refills after a hurricane, flood, earthquake, fire, or other disaster <click here>.
Withdrawal also can happen if you start taking a new medicine or other product, such as a supplement or herb, that causes your body to digest and use up, or "metabolize", your opioid medicine much more quickly. This is called a "drug interaction" and is one reason why all of your healthcare providers need to know that you are taking opioids before they prescribe any new medicines or recommend other products for you.
Opioid withdrawal is not harmful or life threatening, but it can be very unpleasant and even painful. Going through opioid withdrawal is somewhat like having a bad case of the flu. It can take 6 hours or much longer after reducing or stopping an opioid medicine, or starting a new medicine or product that interacts with the opioid, before withdrawal starts. The amount of discomfort, and how long it lasts, depends on the type of opioid medicine that was taken, how long it was used, and the dose.
Here is what to watch for...
Symptoms & Signs of Opioid Withdrawal |
|
|
|
|
Everyone does not experience all of these effects during opioid withdrawal, at all times, or to the same extent. |
|
It is important to understand that tolerance and withdrawal are not signs of addiction in a person who is taking opioid medicine correctly, as prescribed for pain. If your medicine seems to become less effective in relieving pain, or you experience opioid withdrawal at any time, even mild discomfort, contact your opioid prescriber. Never take extra opioid medicine on your own.
E. What is an opioid treatment agreement?
 Opioid pain relievers can be dangerous if they are misused or are used by persons for whom they were not prescribed. Therefore, you are expected to take some of the responsibility for opioid safety. Your opioid prescriber may have you read and sign a "treatment agreement" that lists the things you are expected to do. These are like "Rules of the Road" for using opioid medicines. Even if you are not asked to sign a formal paper, for your own safety and the protection of others, you must agree to do the following...
Opioid pain relievers can be dangerous if they are misused or are used by persons for whom they were not prescribed. Therefore, you are expected to take some of the responsibility for opioid safety. Your opioid prescriber may have you read and sign a "treatment agreement" that lists the things you are expected to do. These are like "Rules of the Road" for using opioid medicines. Even if you are not asked to sign a formal paper, for your own safety and the protection of others, you must agree to do the following...
- Only get prescriptions for pain medicine from one healthcare provider. This person must be told of your medical history, all medicines you are taking (including over-the-counter products, vitamins, or herbs), and about any present or past substance-use problems, including alcohol abuse, in you or in close family members.
- Always get prescriptions filled for pain medicines at the same pharmacy or other approved source. If you must get opioid medicine anywhere else, such as in an emergency or from a dentist, you must tell the healthcare provider who originally prescribed opioids for you.
- All other healthcare providers should be told of the pain medicines you are taking and who is prescribing them for you. If asked, you should allow all of your healthcare providers to share information about your treatment with each other.
 Protect your pain medicine as you would your money or jewelry. At all times, keep the medicine in a safe and out-of-the-way place - locked up if possible.
Protect your pain medicine as you would your money or jewelry. At all times, keep the medicine in a safe and out-of-the-way place - locked up if possible.- Always take opioid medicine only as directed by the prescriber. Never change how you take the medicine, in any way, or take other medicines without first asking the healthcare provider who prescribed your opioids.
 Never use opioid medicines to help you sleep, or combine opioids with any sleep-aid drugs, such as tranquilizers or sedatives.
Never use opioid medicines to help you sleep, or combine opioids with any sleep-aid drugs, such as tranquilizers or sedatives.- Do not drive a car or operate dangerous equipment while taking opioids until you know how you react to the medicine and your opioid prescriber says it is okay.
 Never use illegal drugs, such as cocaine, heroin, crystal meth ("speed"), or others. Marijuana ("pot"), even where legal, or alcohol - wine, beer, or hard liquor - may not be used without your opioid prescriber's permission.
Never use illegal drugs, such as cocaine, heroin, crystal meth ("speed"), or others. Marijuana ("pot"), even where legal, or alcohol - wine, beer, or hard liquor - may not be used without your opioid prescriber's permission.- Keep all of your appointments with your opioid prescriber as scheduled. At each visit you must honestly report on pain relief, any medicine side effects, and new drugs or other products that you are using.
- If asked, you must allow the testing of your urine, saliva, or blood for drugs that you are taking. You also may be asked to bring to office or clinic visits the unused portions of all drugs that you have been prescribed.
- Only ask for medicine refills during regular office or clinic hours. Early refills or a replacement for lost, stolen, or spoiled opioid medicine may not be allowed, depending on what happened.
 Never share, sell, or trade your pain medicine with anyone. Never use someone else's medicines for pain or any other condition.
Never share, sell, or trade your pain medicine with anyone. Never use someone else's medicines for pain or any other condition.
WARNING: Sharing your opioid medicines with another person - even if it is for their pain or they have a similar prescription of their own - may do them great harm, possibly killing them. Sharing, selling, or trading opioids also is against the law and you could go to jail.
- When you are finished using an opioid prescription, you must immediately dispose of any that is left over in a safe way. See the instructions that came with the prescription, or ask your opioid prescriber or pharmacist for directions. Also, see <here> for opioid-disposal instructions.
For safety's sake, if you do not accept and follow the above rules your healthcare provider may not be willing to prescribe, or to continue prescribing, opioids for your pain. Not following the rules also could indicate that you have an opioid-use problem or addiction that requires separate treatment.
F. What opioid prescribing restrictions should I know about?
All persons with pain deserve to be provided treatments that can help them. At the same time, however, opioid medicines can be harmful drugs and at least two agencies in the United States are concerned with reducing the risks of opioid misuse, addiction, overdose, and deaths. These are the U.S. Drug Enforcement Agency (DEA) and the U.S. Food and Drug Administration (FDA).
 The DEA requires qualifying healthcare providers to be specially licensed to prescribe opioid pain relievers, and there are several restrictions or rules:
The DEA requires qualifying healthcare providers to be specially licensed to prescribe opioid pain relievers, and there are several restrictions or rules:
- For stronger as well as longer-acting opioid medicines,* a prescription personally signed by the healthcare provider is required.
- Unlike for most other medicines, an order for a strong or long-acting opioid* cannot simply be called-in or faxed to the pharmacy, except in certain emergencies.
- State laws may dictate how many day's supply can be ordered in a single prescription for a strong or long-acting opioid medicine.*
In certain cases, up to three 30-day prescriptions for the same strong or long-acting opioid* may be provided to a patient during a single visit. This covers 90 days; however, each prescription must be appropriately dated and they all cannot be filled at the same time. Some states may have additional special requirements, so ask your opioid prescriber.
*The DEA has a Schedule of drugs and assigns opioid pain relievers to either Class II, III, or IV. Stronger and long-acting opioids are in Class II, which has stricter prescribing rules. A list of the DEA Scheduled drugs, by name, can be viewed <here>.
The Food and Drug Administration (FDA) is concerned with drug safety. For certain opioid medicines, the FDA requires the manufacturers to develop what are called "REMS" - Risk Evaluation and Mitigation Strategies. These are a set of rules for the particular opioid product that prescribers and patients must follow to help reduce risks of opioid misuse, addiction, and overdose.
For example, opioid prescribers may be required to be sure that a patient might be helped by the particular opioid being prescribed and register the patient to receive it. The patient may need to show that he/she understands how to use the opioid medicine correctly and safely.
Each REMS program is different and REMS for various opioid medicines are still being developed. You should ask your opioid prescriber about any restrictions concerning the opioid that you are being prescribed.
![]() A list of medications, including opioids, with approved REMS programs can be viewed at the FDA's website <here>.
A list of medications, including opioids, with approved REMS programs can be viewed at the FDA's website <here>.
Go to the next section:
3. How can I prevent problems with opioids? <click here>






 Intoxicated behavior - confusion, slurred speech, stumbling.
Intoxicated behavior - confusion, slurred speech, stumbling. Person cannot be aroused or wakened, or is unable to talk if awakened.
Person cannot be aroused or wakened, or is unable to talk if awakened.